Public health officials love a good mystery. They look at the flatlining rates of new HIV infections in the United States and scratch their heads, blaming "stigma," "lack of awareness," or "systemic barriers." They treat the persistence of the epidemic as a tragic puzzle that more money and more "outreach" will eventually solve.
They are wrong. The failure to end the HIV epidemic in America isn't a bug in the system. It is a feature of a multi-billion-dollar bureaucracy that has become too big, too slow, and too comfortable to actually finish the job. We have the tools to stop HIV transmission today. We’ve had them for years. The reason we haven’t succeeded is that the "Ending the HIV Epidemic" (EHE) initiative is addicted to the process of fighting the disease, rather than the result of eliminating it.
The PrEP Paradox and the Gatekeeper Problem
The standard narrative claims PrEP (Pre-Exposure Prophylaxis) isn't reaching the people who need it because of a lack of education. That's a convenient lie. The people at highest risk know exactly what PrEP is. The problem is that we’ve built a medical-industrial gauntlet that makes staying on the drug a part-time job.
To get a pill that is 99% effective at preventing HIV, the CDC guidelines traditionally require a clinic visit every three months for lab work. If you miss an appointment because you work two jobs or lack reliable transport, your prescription lapses. You are then back at square one, vulnerable. We treat a preventative medication like it's a controlled substance.
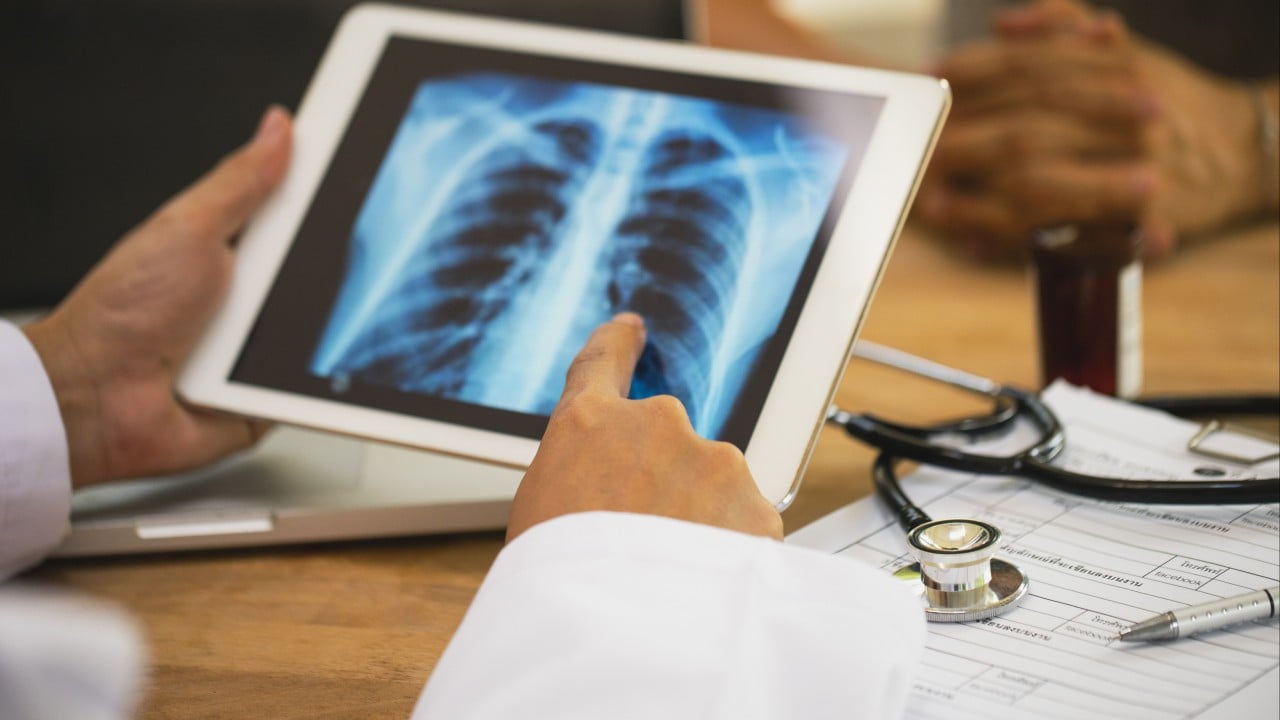
[Image of the HIV replication cycle]
Compare this to the way we handle other public health crises. When we want to stop a regular flu, we put shots in pharmacies and grocery stores. When we want to stop HIV, we demand a battery of blood tests and a sit-down interview with a provider every 90 days. This "clinical-first" model is a relic of the 1990s. By insisting that PrEP remain tethered to the traditional doctor's office, we ensure that the most marginalized populations—the ones the "experts" claim to care about—are the first ones to drop out of care.
The Myth of Underfunding
Every year, advocates march on Washington to demand more funding. They point to the $28 billion plus the U.S. spends annually on HIV/AIDS as if it’s a down payment. In reality, that mountain of cash is exactly what’s blocking progress.
The money flows into a self-perpetuating ecosystem of NGOs, consultants, and health departments. These organizations are funded based on their ability to manage the epidemic, not their ability to make themselves obsolete. If HIV disappeared tomorrow, thousands of "program coordinators" and "diversity consultants" would be out of work.
I have seen city health departments sit on millions in federal grants because they couldn't figure out how to navigate their own procurement rules, while local grassroots clinics—the ones actually seeing the patients—begged for basic supplies. We don't have a funding gap; we have a distribution disaster. We are over-funding the bureaucracy and under-funding the actual delivery of medicine.
U=U is a Policy Tool, Not Just a Slogan
"Undetectable = Untransmittable" (U=U) is the most powerful weapon we have. If every person living with HIV in the U.S. achieved viral suppression, the epidemic would end. Period. The science is settled.
Yet, our policy response is still focused on "awareness" campaigns that look like they were designed by a mid-tier advertising agency in 2005. We spend millions on billboards telling people to "get tested" without fixing the reason they don't stay in treatment: the cost of living.
If you are choosing between a $500 rent hike and a trip to the specialist to check your viral load, the rent wins every time. A contrarian approach would be to stop wasting money on "awareness" and start spending it on direct "adherence support." This means housing vouchers, transportation, and food security tied directly to viral suppression. If we paid for the stability of the patient, the virus would take care of itself. But that doesn't fit the "medical" model, so it gets ignored.
The Rural Blind Spot and the Southern Strategy Failure
The epidemic has shifted. It is no longer a big-city problem centered in New York or San Francisco. It is a Southern, rural, and suburban crisis. Yet, the leadership and the strategy remain firmly rooted in the urban Northeast.
The "Ending the HIV Epidemic" plan targets 57 priority jurisdictions. It’s a heat map of where the virus was five years ago, not where it’s going. While we pour resources into Atlanta and Miami, the rural South is becoming a desert of care. We are fighting a 21st-century viral spread with a 20th-century map.
The "lazy consensus" says we need more "culturally competent" messaging in the South. What we actually need are mobile vans that can dispense meds and draw labs on a dirt road at 7:00 PM. We need to bypass the hospital systems entirely. The virus is fast and adaptive; our public health response is a barge trying to turn in a bathtub.
Stop Testing, Start Treating
The "Test and Link" model is broken. We find people, we give them a positive result, and then we hand them a stack of paperwork and tell them to "follow up." The drop-off rate between a positive test and the first prescription is a chasm.
In a high-functioning system, a positive test should result in a 30-day starter pack of ART (Antiretroviral Therapy) being handed over the counter immediately. No waiting for a "confirmatory" specialist appointment three weeks later. No waiting for insurance pre-authorization. We know the drugs work. We know they are safe. Every day a person waits to start treatment is a day they can transmit the virus and a day they can lose hope in the system.
The Pharmaceutical Hostage Situation
We have to talk about the pricing of PrEP and ART. Even with generics entering the market, the list prices are astronomical. The "Patient Assistance Programs" offered by big pharma are not a solution; they are a PR strategy to keep the government from negotiating lower prices.
By allowing the pharmaceutical industry to dictate the terms of access, the U.S. government has effectively outsourced its public health strategy to entities that profit from the continued existence of the disease. True disruption would mean the government manufacturing its own generic PrEP—something it has the legal authority to do under "march-in rights" for federally funded research—and distributing it for free, by mail, to anyone who wants it.
The Logic of Elimination
If we actually wanted to end the epidemic, the plan would be simple, brutal, and efficient:
- Ditch the 3-month PrEP check-up. Move to annual labs and mail-order delivery.
- Nationalize the ART supply. Remove the profit motive from the "last mile" of delivery.
- Hyper-localize the funding. Strip money from state health departments that fail to hit suppression targets and give it directly to community-led clinics.
- Immediate Treatment Initiation. A positive test is the prescription. No exceptions.
The "HIV Industrial Complex" will tell you this is too risky. They will talk about "patient safety" and "clinical oversight." Don't believe them. They are protecting their budgets, not the patients. We are currently losing the war because we are too afraid to fire the generals who have been failing for forty years.
Stop asking why the epidemic hasn't ended. It hasn't ended because we've built a system that is designed to manage it, not kill it. If you want to stop HIV, you have to stop the bureaucracy first.
Direct the funds to the pharmacy, not the "consultant." Put the pills in the mail, not behind a specialist's gate. If the system won't change, bypass it.